The Most Common Precancer
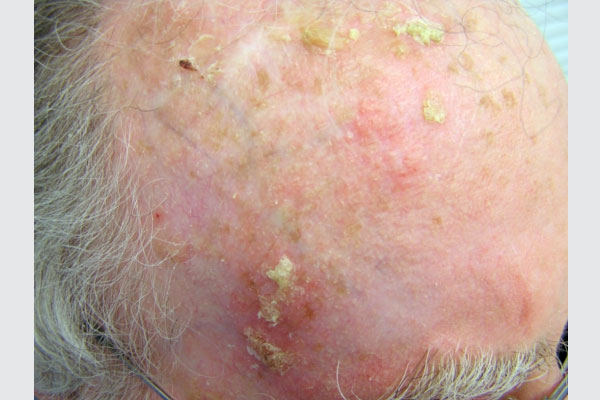 Scaly or crusty growths (lesions) caused by damage from the sun’s ultraviolet (UV) rays, actinic keratosis (AK) is also known as solar keratoses. They typically appear on sun-exposed areas such as the face, bald scalp, lips, and the back of the hands, and are often elevated, rough in texture, and resemble warts. Most become red, but some will be tan, pink, red, and/or flesh-toned. Untreated AKs can advance to squamous cell carcinoma (SCC), the second most common form of skin cancer, and some experts believe they are actually the earliest stage of SCC.
Scaly or crusty growths (lesions) caused by damage from the sun’s ultraviolet (UV) rays, actinic keratosis (AK) is also known as solar keratoses. They typically appear on sun-exposed areas such as the face, bald scalp, lips, and the back of the hands, and are often elevated, rough in texture, and resemble warts. Most become red, but some will be tan, pink, red, and/or flesh-toned. Untreated AKs can advance to squamous cell carcinoma (SCC), the second most common form of skin cancer, and some experts believe they are actually the earliest stage of SCC.
This figure is generally accepted as the best current estimate of the number of Americans with actinic keratosis (AK). People with a fair complexion, blond or red hair, and blue, green or grey eyes (Identify Your Skin Type) have a high likelihood of developing one or more of these common precancers if they spend time in the sun and live long enough. Location makes a difference: The closer to the equator you live, the more likely you are to have actinic keratoses. The incidence is slightly higher in men, because they tend to spend more time in the sun and use less sun protection than women do. African-Americans, Hispanics, Asians and others with darker skin are not as susceptible as Caucasians (Skin Cancer and Skin of Color).
What Is It?
An actinic keratosis, also known as a solar keratosis, is a scaly or crusty growth (lesion). It most often appears on the bald scalp, face, ears, lips, backs of the hands and forearms, shoulders, neck or any other areas of the body frequently exposed to the sun. You’ll most often see the plural, “keratoses,” because there is seldom just one. In the beginning, actinic keratoses are frequently so small that they are recognized by touch rather than sight. It feels as if you were running a finger over sandpaper. There are many times the number of invisible (subclinical) lesions as visible ones on the skin surface.
Most often, actinic keratoses develop slowly and reach a size from an eighth to a quarter of an inch. Early on, they may disappear only to reappear later. Most become red, but some will be light or dark tan, pink, red, a combination of these, or the same color as your skin. Occasionally they itch or produce a pricking or tender sensation. They can also become inflamed and surrounded by redness. In rare instances, actinic keratoses can even bleed. If you have actinic keratoses, it indicates that you have sustained sun damage and could develop any kind of skin cancer — not just squamous cell carcinoma.
Is there cause for concern?
Actinic keratosis can be the first step leading to squamous cell carcinoma and is therefore known as a “precancer.” Although the vast majority of actinic keratoses remain benign, some studies report that up to ten percent may advance to squamous cell carcinoma. This percentage does not sound very large, but it has a large impact. When it comes to squamous cell carcinomas, 40-60 percent begin as untreated actinic keratoses and may advance to invade the surrounding tissues. About 2 to 10 percent of these squamous cell carcinomas spread to the internal organs and are life-threatening.
Another form of actinic keratosis, actinic cheilitis, develops on the lips and may evolve into squamous cell carcinoma. The more keratoses you have, the greater the chance that one or more may turn into skin cancer. In fact, some scientists interpret actinic keratosis as the earliest form of squamous cell carcinoma.
Treatment Options
Photodynamic Therapy (PDT) PDT can be especially useful for lesions on the face and scalp. Topical 5-aminolevulinic acid (5-ALA), a photosensitizing agent, is applied to the lesions. Subsequently, the medicated area is exposed to strong light that activates 5-ALA. The treatment selectively destroys actinic keratoses, causing little damage to surrounding normal skin, although some swelling and redness often occur.
Topical Medications Medicated creams and solutions are very effective by themselves or in combination with another form of treatment when a person has many actinic keratoses.
5-fluorouracil (5-FU) ointment or liquid in concentrations from 0.5 to 5 percent has FDA approval and is the most widely used topical treatment for actinic keratoses. It is effective against not only the surface lesions but also the subclinical ones. Rubbed gently onto the lesions once or twice a day for two to four weeks, it produces cure rates of up to 93 percent. Reddening, swelling and crusting may occur, but they are temporary. The lesions usually heal within two weeks of stopping treatment. There is rarely scarring and the cosmetic result is good.
Imiquimod 5% cream, also FDA-approved, works in a different way: It stimulates the immune system to produce interferon, a chemical that destroys cancerous and precancerous cells. It is rubbed gently on the lesion twice a week for four to sixteen weeks. The cream is generally well-tolerated, but some individuals develop redness and ulcerations.
Diclofenac is a non-steroidal anti-inflammatory drug used in combination with hyaluronic acid, a chemical found naturally in the body. The resulting gel is applied twice a day for two to three months. The diclofenac prevents an inflammatory response, so this topical is well-tolerated, and the hyaluronic acid delays uptake of the diclofenac, leading to higher concentrations in the skin. It is used in persons who are oversensitive to other topical treatments.
Ingenol mebutate is a topical gel approved by the FDA for AK treatment in 2012. The gel, used in 0.015% or 0.05% concentrations depending on the AK site, is the first topical therapy to effectively treat AKs in just two or three days. The 0.015% gel is applied to the face and scalp once a day for three consecutive days, and the more concentrated 0.05% gel is applied to the trunk and extremities once a day for two consecutive days. The most common side effects are skin redness, flaking/scaling, crusting and swelling.
Cryosurgery This is the most commonly used treatment method when a limited number of lesions exist. No cutting or anesthesia is required. Liquid nitrogen, applied with a spray device or cotton-tipped applicator, freezes the growths. The lesions subsequently shrink or become crusted and fall off. Temporary redness and swelling may occur after treatment, and in some patients, white spots may remain permanently.
Combination Therapies If one form of therapy is good, two may be better; some of the treatment options described here are especially effective when used together or in sequence. This approach can both improve the cure rate and reduce side effects. One to two weeks of 5-FU followed by cryosurgery can reduce the healing time for 5-FU and decrease the likelihood of white spots following cryosurgery.
Chemical Peeling This method, best known for reversing the signs of photoaging, is also used to remove some actinic keratoses on the face. Trichloroacetic acid (TCA) and/or similar chemicals are applied directly to the skin. The top skin layers slough off and are usually replaced within seven days. This technique requires local anesthesia and can cause temporary discoloration and irritation.
Laser Surgery A carbon dioxide or erbium YAG laser is focused onto the lesion, and the beam cuts through tissue without causing bleeding. This is a good option for lesions in small or narrow areas, and, therefore, can be particularly effective for keratoses on the face and scalp, as well as actinic cheilitis on the lips. However, local anesthesia may be necessary, and some pigment loss can occur. Lasers are useful for people taking blood thinners or as a secondary treatment when others have not succeeded.
What Causes Actinic Keratosis
Chronic sun exposure is the cause of almost all actinic keratoses. Sun damage to the skin is cumulative, so even a brief period in the sun adds to the lifetime total. Cloudy days aren’t safe either, because 70-80 percent of solar ultraviolet (UV) rays can pass through clouds. These harmful rays can also bounce off sand, snow and other reflective surfaces, giving you extra exposure.
The ultraviolet radiation given off by the lamps in a tanning salon can be even more dangerous than the sun, so dermatologists warn against indoor tanning. Occasionally, actinic keratoses may be caused by extensive exposure to X-rays or a number of industrial chemicals.
What Age Has to Do with It
Because the total amount of time spent in the sun adds up year by year, older people are most likely to develop actinic keratoses. However, nowadays, some individuals in their 20s are affected. Still, actinic keratoses become much more common in people over the age of 50. Some experts believe almost everyone over 80 has actinic keratoses.
Also, individuals whose immune defenses are weakened by cancer chemotherapy, AIDS, organ transplantation or excessive UV exposure are less able to fight off the effects of the radiation and thus more likely to develop actinic keratoses.
Why Is It Treated?
While actinic keratosis is the most common precancer, not all keratoses turn into cancers. Unfortunately, there is no way to know ahead of time which actinic keratoses are precursors of squamous cell carcinoma. That is why it is fortunate that there are so many effective treatments for eliminating actinic keratoses.
When an actinic keratisis is suspected to be an early cancer, the physician may take tissue for biopsy. This is done by shaving off the top of the lesion with a scalpel or scraping it off with a curette. Local anesthesia is required. Bleeding is usually stopped with a styptic agent.
How to Recognize Actinic Keratosis
Examples of typical actinic keratoses are shown here, so examine your skin regularly for lesions that look like them. But it’s not always that simple: Many actinic keratoses have quite a different appearance, so if you find any unusual or changing growth, be suspicious and see your doctor promptly.
How to Prevent Actinic Keratosis
The best way to prevent actinic keratosis is to protect yourself from the sun. Here are some sun-safety habits that really work.
- Seek the shade, especially between 10 AM and 4 PM.
- Do not burn.
- Use a broad spectrum (UVA/UVB) sunscreen with an SPF of 15 or higher every day. For extended outdoor activity, use a water-resistant, broad spectrum (UVA/UVB sunscreen with an SPF of 30 or higher.
- Apply 1 ounce (2 tablespoons) of sunscreen to your entire body 30 minutes before going outside. Reapply every two hours or immediately after swimming or excessive sweating.
- Cover up with clothing, including a broad-brimmed hat and UV-blocking sunglasses.
- Keep newborns out of the sun. Sunscreens should be used on babies over the age of six months.
- Examine your skin head-to-toe every month.
- See your doctor every year for a professional skin exam.
- Avoid tanning and UV tanning booths.

