SERVICES
- Allergy Screening
- Chemical Peels
- Dermapen
- Facial Skin Analysis
- FreshEyes
- Hyperhidrosis (Excessive Sweating)
- Hair Loss Treatment
- Laser Clinic
- Liquid Facelift
- Keloid Treatments
- Medical Facials
- Medical Treatments
- Mole Mapping
- Photodynamic Therapy (PDT)
- Skincare Advice
- Pigmentation Treatment
- Surgical Procedures
- Ultraviolet Phototherapy
USEFUL LINKS
What are urticaria and angioedema?
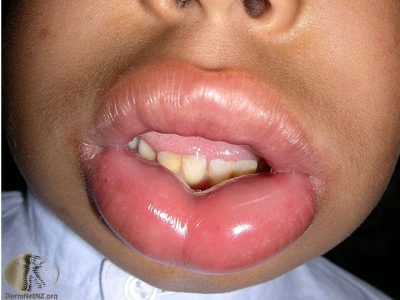 Urticaria is common, and affects about 20% of people at some point in their lives. It is also known as hives or nettle rash. The short-lived swellings of urticaria are known as weals (see below). Angioedema is a deeper form of urticaria.
Urticaria is common, and affects about 20% of people at some point in their lives. It is also known as hives or nettle rash. The short-lived swellings of urticaria are known as weals (see below). Angioedema is a deeper form of urticaria.
An affected individual may have urticaria alone, or angio-oedema alone, or both together. The most common form is called ‘ordinary urticaria’, which is usually divided into ‘acute’ and ‘chronic’ forms. In ‘acute’ urticaria/angio-oedema, the episode lasts from a few days up to six weeks. Chronic urticaria, by definition, lasts for more than six weeks. Other less common types of urticaria are described later in this leaflet. Also included is urticarial vasculitis (in which an inflammation of the blood vessels causes an urticaria-like rash, and is therefore different from normal urticaria).
What causes urticaria and angio-oedema?
Both are caused by the release of histamine from cells in the skin called mast cells. This can be triggered in many ways, for example by exercise, by pressure on the skin, and by other physical factors, as well as by foods, drugs and infections. However in the common ‘ordinary’ form of urticaria and angio-oedema, it is unusual for an external cause to be identified. In some patients with ordinary chronic urticaria, the release of histamine from skin mast cells is triggered by factors circulating in the blood, such as antibodies directed against their own mast cells – a process known as autoimmunity. Tests for this are not routinely available, and generally do not alter the treatments used.
Often no cause for acute urticaria can be found, but sometimes it may be caused by infections such as a cold, influenza or a sore throat. Almost any medicine can cause ‘acute’ urticaria, but painkillers (especially aspirin and medicines like ibuprofen), antibiotics (especially penicillins) and vaccinations are most likely to be responsible. Angio-oedema, in particular, can be caused by a type of drug (ACE inhibitors) used to treat high blood pressure. Foods are not usually the cause of acute urticaria, although occasionally nuts, fish, tomatoes, vegetables and berries may be responsible
What are the symptoms of urticaria and angio-oedema?
The main symptom of urticaria is itch: angio-oedema, however, is not usually itchy. Although urticaria can be distressing, because of the itching and its appearance, it has no direct effect on general health. Rarely, the swelling of angio-oedema may affect the tongue or throat, causing difficulty with breathing or swallowing. This can be alarming but rarely life-threatening, except in acute food or medicine allergies and the rare hereditary form of angio-oedema.
Are urticaria and angio-oedema hereditary?
The ‘ordinary’ common type of urticaria and angio-oedema is not hereditary.
What do ordinary urticaria and angio-oedema look like?
The weals of urticaria may be flesh-coloured, pink or red. They can be of different shapes and sizes, but usually look like nettle stings. An important feature of urticaria is that individual lesions usually disappear within a day, and often last only a matter of hours. However, they sometimes leave bruising especially in children. New weals may then appear in other areas. In ordinary urticaria, the weals can occur anywhere on the body, at any time.
The pale or pink, deeper swellings of angio-oedema occur most frequently on the eyelids, lips and sometimes in the mouth, but they may occur anywhere. They are not usually itchy, and tend to settle within a few days. If the hands and feet are affected, they may feel tight and painful.
How will ordinary urticaria be diagnosed?
Usually its appearance, or a description of it, will be enough for your doctor to make the diagnosis. In the vast majority of people no cause can be found, though your doctor will ask you questions to try to identify one. There is no special test that can reliably identify the cause of urticaria, but some tests may be done if your answers suggest an underlying cause.
In acute urticaria, investigation is usually unnecessary. Occasionally, if an allergic reaction is suspected, a specific blood test, to detect antibodies in the bloodstream, or a skin prick test may be performed by a specialist in skin or allergic disease. In chronic urticaria, it is rare for allergy to be the cause, so routine allergy tests are not necessary. In a small percentage of people, foods, colouring agents and preservatives appear to worsen the urticaria, and it might be helpful to keep a food diary: these substances can be left out of the diet to see if the condition improves, and later deliberately reintroduced to confirm whether they are the cause of the urticaria. However, as urticaria is such a fluctuating disease, this is not always accurate and will not always show you definitely what is causing the problem.
Can ordinary urticaria and angio-oedema be cured?
The treatments outlined below suppress the condition rather than cure it. In half of the people with chronic ordinary urticaria, the rash lasts for 6-12 months, and then gradually disappears, although it can last considerably longer. It usually does not return. However, in any one individual the course of urticaria is unpredictable.
What is the treatment for ordinary urticaria?![]() It is important to avoid anything that may worsen urticaria. These are listed below in detail under the heading ‘What can I do?’
It is important to avoid anything that may worsen urticaria. These are listed below in detail under the heading ‘What can I do?’![]() Antihistamines block the effect of histamine, and reduce itching and the rash in most people, but may not relieve urticaria completely. If urticaria occurs frequently, it is best to take antihistamines regularly. There are many different types. The older ones often cause drowsiness. The newer ones are much less likely to cause drowsiness, but may do so if taken with alcohol. No particular antihistamine is best for everyone, so your doctor may need to try different ones to find the one that suits you best. Antihistamine tablets may need to be taken for as long as the urticaria persists. Reports of serious side effects are very rare, but occasionally a few cause weight gain, and some should not be taken at the same time as particular medicines.
Antihistamines block the effect of histamine, and reduce itching and the rash in most people, but may not relieve urticaria completely. If urticaria occurs frequently, it is best to take antihistamines regularly. There are many different types. The older ones often cause drowsiness. The newer ones are much less likely to cause drowsiness, but may do so if taken with alcohol. No particular antihistamine is best for everyone, so your doctor may need to try different ones to find the one that suits you best. Antihistamine tablets may need to be taken for as long as the urticaria persists. Reports of serious side effects are very rare, but occasionally a few cause weight gain, and some should not be taken at the same time as particular medicines.![]() A related type of antihistamine (e.g. cimetidine and ranitidine), which is usually used to treat stomach ulcers, can be added to the standard antihistamines used to treat the skin.
A related type of antihistamine (e.g. cimetidine and ranitidine), which is usually used to treat stomach ulcers, can be added to the standard antihistamines used to treat the skin.![]() Topical preparations such as calamine lotion can be soothing.
Topical preparations such as calamine lotion can be soothing.![]() If antihistamine tablets are not helpful you can discuss this with your doctor who may arrange further tests, and try other medicines. Some of these (such as montelukast, a treatment for asthma) may not be licensed for urticaria, but can be useful treatments.
If antihistamine tablets are not helpful you can discuss this with your doctor who may arrange further tests, and try other medicines. Some of these (such as montelukast, a treatment for asthma) may not be licensed for urticaria, but can be useful treatments.![]() Oral steroids may occasionally be given briefly for severe flares of acute and chronic urticaria, but generally are not necessary.
Oral steroids may occasionally be given briefly for severe flares of acute and chronic urticaria, but generally are not necessary.![]() New treatments that act by suppressing the immune system (e.g. ciclosporin) are being used in a few of the most severely affected people in specialist skin and allergy centres, and may be beneficial.
New treatments that act by suppressing the immune system (e.g. ciclosporin) are being used in a few of the most severely affected people in specialist skin and allergy centres, and may be beneficial.![]() Injections of adrenaline (epinephrine) (which can be self administered) often provide rapid relief, but this form of treatment is only used in the most extreme situations, such as if urticaria or angio-oedema causes breathing problems.
Injections of adrenaline (epinephrine) (which can be self administered) often provide rapid relief, but this form of treatment is only used in the most extreme situations, such as if urticaria or angio-oedema causes breathing problems.
What can I do?![]() It is important to avoid anything that may worsen urticaria, such as heat, tight clothes, alcohol, and aspirin-containing medicines, and if possible other similar medicines such as ibuprofen (paracetamol does not normally cause a problem).
It is important to avoid anything that may worsen urticaria, such as heat, tight clothes, alcohol, and aspirin-containing medicines, and if possible other similar medicines such as ibuprofen (paracetamol does not normally cause a problem).![]() Medicines called ACE inhibitors (often used to treat high blood pressure) should be avoided, especially if angio-oedema is present.
Medicines called ACE inhibitors (often used to treat high blood pressure) should be avoided, especially if angio-oedema is present.![]() Foods, colouring agents and preservatives can be avoided in the rare instances where these have proved to be a problem.
Foods, colouring agents and preservatives can be avoided in the rare instances where these have proved to be a problem.![]() Seek medical advice urgently if you are having problems with breathing or swallowing.
Seek medical advice urgently if you are having problems with breathing or swallowing.![]() Consider the purchase of a Medic Alert bracelet to inform others about your condition in the event of you not being able to do so yourself:
Consider the purchase of a Medic Alert bracelet to inform others about your condition in the event of you not being able to do so yourself:
Other urticarias![]() The physical urticarias Other forms of urticaria are triggered by physical factors such as heat, cold, friction, pressure on the skin and even by water. The weals usually occur within minutes, and last for less than one hour (except delayed pressure urticaria). Physical urticarias usually occur in healthy young adults, and are not uncommon. They may occur in association with ordinary urticaria, or with each other, and tend to improve with time. They include the following types:
The physical urticarias Other forms of urticaria are triggered by physical factors such as heat, cold, friction, pressure on the skin and even by water. The weals usually occur within minutes, and last for less than one hour (except delayed pressure urticaria). Physical urticarias usually occur in healthy young adults, and are not uncommon. They may occur in association with ordinary urticaria, or with each other, and tend to improve with time. They include the following types:![]() Dermographism (“skin writing”) In this type, itchy weals occur after friction such as rubbing or stroking the skin, which is generally very itchy especially when hot.
Dermographism (“skin writing”) In this type, itchy weals occur after friction such as rubbing or stroking the skin, which is generally very itchy especially when hot. ![]() Weals and red marks often appear as lines at the sites of scratching, and generally last for less than one hour. Usually no cause is found.
Weals and red marks often appear as lines at the sites of scratching, and generally last for less than one hour. Usually no cause is found.![]() Cold urticaria Cold, including rain, wind and cold water, causes itching and wealing in chilled areas. Swimming in cold water may cause severe wealing and fainting, and must be avoided. Patients should report their cold urticaria to medical personnel before operations so that, if weals appear during the procedure, cold urticaria can be considered. Usually no cause can be found for cold urticaria.
Cold urticaria Cold, including rain, wind and cold water, causes itching and wealing in chilled areas. Swimming in cold water may cause severe wealing and fainting, and must be avoided. Patients should report their cold urticaria to medical personnel before operations so that, if weals appear during the procedure, cold urticaria can be considered. Usually no cause can be found for cold urticaria.![]() Solar urticaria This is rare. Redness, itching and weals occur on the skin immediately after exposure to sunlight, and last for less than one hour.
Solar urticaria This is rare. Redness, itching and weals occur on the skin immediately after exposure to sunlight, and last for less than one hour.![]() Aquagenic urticaria This is extremely rare. Small weals occur on the skin at the site of contact with water of any temperature, usually on the upper part of the body.
Aquagenic urticaria This is extremely rare. Small weals occur on the skin at the site of contact with water of any temperature, usually on the upper part of the body.![]() Delayed pressure urticaria Swellings occur at skin sites to which pressure has been applied, for example from tight clothes or from gripping tools. Usually the swelling develops several hours later. It can be painful and last longer than a day. People with pressure urticaria nearly always have ordinary urticaria as well. Many of the physical urticarias are improved by avoiding their cause, and regular treatment with antihistamines. However, antihistamines do not usually help delayed pressure urticaria. Sometimes a short course of oral steroids will help if the symptoms of delayed pressure urticaria are very severe.
Delayed pressure urticaria Swellings occur at skin sites to which pressure has been applied, for example from tight clothes or from gripping tools. Usually the swelling develops several hours later. It can be painful and last longer than a day. People with pressure urticaria nearly always have ordinary urticaria as well. Many of the physical urticarias are improved by avoiding their cause, and regular treatment with antihistamines. However, antihistamines do not usually help delayed pressure urticaria. Sometimes a short course of oral steroids will help if the symptoms of delayed pressure urticaria are very severe.![]() Cholinergic urticaria This occurs under conditions that cause sweating, such as exertion, heat, emotional stress and eating spicy food. Within minutes, small itchy bumps with variable redness appear, usually on the upper part of the body but they may be widespread. The weals last for less than one hour, but in severe cases may join together to form larger swellings. Antihistamines usually help, and are sometimes best taken before a triggering event (e.g. exercise).
Cholinergic urticaria This occurs under conditions that cause sweating, such as exertion, heat, emotional stress and eating spicy food. Within minutes, small itchy bumps with variable redness appear, usually on the upper part of the body but they may be widespread. The weals last for less than one hour, but in severe cases may join together to form larger swellings. Antihistamines usually help, and are sometimes best taken before a triggering event (e.g. exercise).![]() Contact urticaria Various chemicals, foods, plants, animals, and animal products, can cause weals within minutes at the site of contact. These weals do not last long. Some of the commoner causes are eggs, nuts (e.g. peanuts), citrus fruits, rubber (latex) and contact with cats and dogs. Although often the reactions are mild, occasionally they can be severe, for example after contact with rubber and peanuts in very sensitive individuals.
Contact urticaria Various chemicals, foods, plants, animals, and animal products, can cause weals within minutes at the site of contact. These weals do not last long. Some of the commoner causes are eggs, nuts (e.g. peanuts), citrus fruits, rubber (latex) and contact with cats and dogs. Although often the reactions are mild, occasionally they can be severe, for example after contact with rubber and peanuts in very sensitive individuals.![]() Angio-oedema without weals Angio-oedema occurring without urticaria can be due to a variety of causes such as medicines (e.g. aspirin, ACE inhibitors) or food allergies. Most commonly it is a component of chronic ordinary urticaria/ angio-oedema, where no cause can be identified.
Angio-oedema without weals Angio-oedema occurring without urticaria can be due to a variety of causes such as medicines (e.g. aspirin, ACE inhibitors) or food allergies. Most commonly it is a component of chronic ordinary urticaria/ angio-oedema, where no cause can be identified.![]() Hereditary angio-oedema This is a very rare form of angio-oedema which tends to run in families. Patients get swellings of the face, mouth, throat, and sometimes of the gut, leading to colic. The condition is due to an inherited deficiency of a blood protein and can be identified by a blood test. It can be treated by medicines to prevent attacks and sometimes by replacing the deficient protein in the blood in an acute attack. A severe attack of hereditary angio-oedema can be life threatening if left untreated; therefore patients may be advised to wear a Medic Alert bracelet to alert physicians in an emergency.
Hereditary angio-oedema This is a very rare form of angio-oedema which tends to run in families. Patients get swellings of the face, mouth, throat, and sometimes of the gut, leading to colic. The condition is due to an inherited deficiency of a blood protein and can be identified by a blood test. It can be treated by medicines to prevent attacks and sometimes by replacing the deficient protein in the blood in an acute attack. A severe attack of hereditary angio-oedema can be life threatening if left untreated; therefore patients may be advised to wear a Medic Alert bracelet to alert physicians in an emergency.![]() Urticarial vasculitis A small percentage of people with urticaria develop weals that last longer than two days. These may be tender and occasionally bruise. People affected with this condition may feel unwell and have joint and stomach pains. This is because their blood vessels become inflamed (a process known as vasculitis). The diagnosis is confirmed by examining under the microscope a small piece of a weal that has been removed. The cause is rarely found, though blood tests are usually undertaken. Antihistamines are not very helpful but other medicines that help inflammation can be used.
Urticarial vasculitis A small percentage of people with urticaria develop weals that last longer than two days. These may be tender and occasionally bruise. People affected with this condition may feel unwell and have joint and stomach pains. This is because their blood vessels become inflamed (a process known as vasculitis). The diagnosis is confirmed by examining under the microscope a small piece of a weal that has been removed. The cause is rarely found, though blood tests are usually undertaken. Antihistamines are not very helpful but other medicines that help inflammation can be used.
Patient Testimonials
EXCELLENTTrustindex verifies that the original source of the review is Google. From my first visit with Dr Jhetam I knew I would go back. He is compassionate , friendly and has an interaction which made you feel comfortable. This is very important in any doctor because our relationship with our doctor is very intimate.Posted onTrustindex verifies that the original source of the review is Google. Dr Jhetman is truly one of a kind. Anyone who is fortunate enough to be in his care can so grateful. Academic, informative and reassuring. It’s hard to find a doctor who has this combination of skills these days. He dealt with my Melonoma concerns with swift and professional care. And his staff are equally as competent and caring. I cannot commend Dr Jhetman and his staff enough on true patient care. Thank you!Posted onTrustindex verifies that the original source of the review is Google. I was absolutely satisfied with my experience with Dr Jhetham & his winning team. Keep up the good work.Posted onTrustindex verifies that the original source of the review is Google. Best skin doctor..Dr Jetham prescribed the best products that have brought so much of a glow to my skin..being a transplant patient and so much happening to my skin just 4 visits to him and my face is back to it's radiance ..I hightly reccomend Dr Jetham ...you won't go wrong..Posted onTrustindex verifies that the original source of the review is Google. Dr. Imraan Jhetam and his team provided exceptional care, showcasing professionalism and compassion in every interaction. Dr. Jhetam took the time to thoroughly explain everything, addressing each of my concerns with empathy and understanding. My experience with him was truly wonderful, and I highly appreciate his dedication to patient care.Verified by TrustindexTrustindex verified badge is the Universal Symbol of Trust. Only the greatest companies can get the verified badge who has a review score above 4.5, based on customer reviews over the past 12 months. Read more